re-write def'n, needs attention of an expert.... |
m small fixes, sub-divide etiology, +pseudomembrane |
||
| Line 14: | Line 14: | ||
MeshNumber = C06.405.205.265 | |
MeshNumber = C06.405.205.265 | |
||
}} |
}} |
||
In [[medicine]], '''colitis''' ([[plural|pl]] |
In [[medicine]], '''colitis''' ([[plural|pl.]] colitides) refers to an [[inflammation]] of the [[colon (anatomy)|colon]] or, less precisely, an inflammation of the [[large intestine]]. Colitides may be [[acute]] and self-limited or [[Chronic (medical)|chronic]]. They broadly fit into the category of [[digestive diseases|digestive disease]]s. |
||
Causes for colitis include infections and [[autoimmunity|autoimmune disorders]]. A common chronic cause of colitis is [[inflammatory bowel disease]] (IBD), which should not to be confused with [[irritable bowel syndrome]] (IBS). |
Causes for colitis include infections, chemical ingestions and [[autoimmunity|autoimmune disorders]]. A common chronic cause of colitis is [[inflammatory bowel disease]] (IBD), which should not to be confused with [[irritable bowel syndrome]] (IBS). |
||
==Signs and symptoms== |
==Signs and symptoms== |
||
The [[sign (medicine)|signs]] and [[symptom]]s of colitides are quite variable and dependent on the etiology of the given colitis and factors that influence its course and severity. |
|||
Symptoms and signs of a colitis may include intense [[pain]], tenderness in the abdomen, [[Clinical depression|depression]], rapid weight loss, aches and pains within the joints, loss of appetite, [[Fatigue (medical)|fatigue]], changes in bowel habits (increased frequency), [[fever]]; swelling of the colon tissue, [[erythema]] (redness) of the surface of the colon, [[Peptic ulcer|ulcers]] on the colon (in [[ulcerative colitis]]) which can [[bleeding|bleed]], mucus in the [[Human feces|stool]], blood in stool and rectal bleeding. [[Diarrhea]] may present itself, although some forms of colitis are [[constipation]] so the stool and bowel movements can appear normal. |
|||
Other symptoms may include: gas, bloating, indigestion, heartburn, reflux, [[Gastroesophageal reflux disease|Gastro esophageal reflux disease]] (GERD, or GORD when using the [[Commonwealth spelling]] ''oesophageal''), cramps, urgency and many other uncomfortable aches in the gastrointestinal system. |
Other symptoms may include: gas, bloating, indigestion, heartburn, reflux, [[Gastroesophageal reflux disease|Gastro esophageal reflux disease]] (GERD, or GORD when using the [[Commonwealth spelling]] ''oesophageal''), cramps, urgency and many other uncomfortable aches in the gastrointestinal system. |
||
| Line 59: | Line 61: | ||
==Types== |
==Types== |
||
There are many types of colitides. They are usually classified by the etiology. |
|||
Types of colitis include [[ulcerative colitis]] (UC), [[Crohn's disease|Crohn's colitis]], [[diversion colitis]], [[ischemic colitis]], infectious colitis, fulminant colitis, [[collagenous colitis]], [[chemical colitis]], [[microscopic colitis]], [[lymphocytic colitis]], and [[atypical colitis]]. |
|||
Types of colitis include: |
|||
===Autoimmune=== |
|||
*Inflammatory bowel disease. |
|||
**[[Ulcerative colitis]] (UC), |
|||
**[[Crohn's disease|Crohn's disease]], |
|||
===Idiopathic=== |
|||
*[[Microscopic colitis]], |
|||
**[[Lymphocytic colitis]], |
|||
**[[Collagenous colitis]], |
|||
===Iatrogenic=== |
|||
*[[Diversion colitis]], |
|||
*[[Chemical colitis]], |
|||
===Vascular disease=== |
|||
*[[Ischemic colitis]], |
|||
===Infectious=== |
|||
[[Image:Colonic pseudomembranes low mag.jpg|thumb|right|[[Micrograph]] of a [[colon (anatomy)|colonic]] pseudomembrane in ''[[Clostridium difficile]]'' colitis, a type of [[pseudomembranous colitis]].]] |
|||
*Infectious colitis, |
|||
A well-known subtype of infectious colitis is [[pseudomembranous colitis]], which results from infection by a [[toxigenic]] strain of ''[[Clostridium difficile]]'' (c-diff).<ref>{{cite web |
A well-known subtype of infectious colitis is [[pseudomembranous colitis]], which results from infection by a [[toxigenic]] strain of ''[[Clostridium difficile]]'' (c-diff).<ref>{{cite web |
||
| Line 74: | Line 99: | ||
| doi = |
| doi = |
||
| accessdate = 2006-09-15}}</ref> |
| accessdate = 2006-09-15}}</ref> |
||
| ⚫ | |||
| ⚫ | Entero[[hemorrhagic]] colitis may be caused by [[Shiga toxin]] in ''[[Shigella dysenteriae]]'' or ''Shigatoxigenic group'' of ''[[Escherichia coli]]'' (STEC), which includes [[serotype]] [[Escherichia coli O157:H7|O157:H7]] and other enterohemorrhagic ''E. coli''.<ref name=Beutin_2006>{{cite journal |author=Beutin L |title=Emerging enterohaemorrhagic Escherichia coli, causes and effects of the rise of a human pathogen |journal=J Vet Med B Infect Dis Vet Public Health |volume=53 |issue=7 |pages=299–305 |year=2006 |pmid=16930272}}</ref> |
||
| ⚫ | |||
===Waste-basket=== |
|||
*Atypical colitis |
|||
===Severity of colitides=== |
|||
*Fulminant colitis. |
|||
Any colitis with a rapid downhill clinical course{{Clarify|date=September 2009}} is known as ''fulminant colitis''. In addition to the [[diarrhea]], [[fever]], and [[anemia]] seen in colitis, the patient has severe abdominal pain and presents a clinical picture similar to that of [[septicemia]], where [[Shock (circulatory)|shock]] is present. Approximately half of these patients require surgery. |
Any colitis with a rapid downhill clinical course{{Clarify|date=September 2009}} is known as ''fulminant colitis''. In addition to the [[diarrhea]], [[fever]], and [[anemia]] seen in colitis, the patient has severe abdominal pain and presents a clinical picture similar to that of [[septicemia]], where [[Shock (circulatory)|shock]] is present. Approximately half of these patients require surgery. |
||
[[Irritable bowel syndrome]], a separate disease, has been called spastic colitis or spastic colon. This name causes confusion, since colitis is not a feature of irritable bowel syndrome. |
[[Irritable bowel syndrome]], a separate disease, has been called spastic colitis or spastic colon. This name causes confusion, since colitis is not a feature of irritable bowel syndrome. |
||
| ⚫ | Entero[[hemorrhagic]] colitis may be caused by [[Shiga toxin]] in ''[[Shigella dysenteriae]]'' or ''Shigatoxigenic group'' of ''[[Escherichia coli]]'' (STEC), which includes [[serotype]] [[Escherichia coli O157:H7|O157:H7]] and other enterohemorrhagic ''E. coli''.<ref name=Beutin_2006>{{cite journal |author=Beutin L |title=Emerging enterohaemorrhagic Escherichia coli, causes and effects of the rise of a human pathogen |journal=J Vet Med B Infect Dis Vet Public Health |volume=53 |issue=7 |pages=299–305 |year=2006 |pmid=16930272}}</ref> |
||
==Treatment== |
==Treatment== |
||
How a given colitis is treated is dependent on its etiology. |
|||
Treatment of colitis may include the administration of [[antibiotic]]s, [[Azathioprine]] or similar [[immunosupressant]]s; [[glucocorticoids|steroids]] such as [[prednisolone]] and [[prednisone]]; one or several of a number of other drugs that ameliorate inflammation and pain ([[buscopan]]). As it is a chronic condition the objective is "remission" rather than cure. |
Treatment of colitis may include the administration of [[antibiotic]]s, [[Azathioprine]] or similar [[immunosupressant]]s; [[glucocorticoids|steroids]] such as [[prednisolone]] and [[prednisone]]; one or several of a number of other drugs that ameliorate inflammation and pain ([[buscopan]]). As it is a chronic condition the objective is "remission" rather than cure. |
||
Revision as of 05:06, 9 December 2009
| Colitis | |
|---|---|
| Specialty | Gastroenterology |
In medicine, colitis (pl. colitides) refers to an inflammation of the colon or, less precisely, an inflammation of the large intestine. Colitides may be acute and self-limited or chronic. They broadly fit into the category of digestive diseases.
Causes for colitis include infections, chemical ingestions and autoimmune disorders. A common chronic cause of colitis is inflammatory bowel disease (IBD), which should not to be confused with irritable bowel syndrome (IBS).
Signs and symptoms
The signs and symptoms of colitides are quite variable and dependent on the etiology of the given colitis and factors that influence its course and severity.
Symptoms and signs of a colitis may include intense pain, tenderness in the abdomen, depression, rapid weight loss, aches and pains within the joints, loss of appetite, fatigue, changes in bowel habits (increased frequency), fever; swelling of the colon tissue, erythema (redness) of the surface of the colon, ulcers on the colon (in ulcerative colitis) which can bleed, mucus in the stool, blood in stool and rectal bleeding. Diarrhea may present itself, although some forms of colitis are constipation so the stool and bowel movements can appear normal.
Other symptoms may include: gas, bloating, indigestion, heartburn, reflux, Gastro esophageal reflux disease (GERD, or GORD when using the Commonwealth spelling oesophageal), cramps, urgency and many other uncomfortable aches in the gastrointestinal system.
Common tests which reveal these signs include X-rays of the colon, testing the stool for blood and pus, sigmoidoscopy, and colonoscopy. Additional tests include stool cultures and blood tests, including blood chemistry tests. A high erythrocyte sedimentation rate (ESR) is one typical finding in acute exacerbations of colitis.
Food triggers
Many people have found that one or more of the following foods can trigger their symptoms [1]:
- alcohol
- caffeine
- carbonated beverages
- dairy products, if lactose intolerant
- dried beans, peas, and legumes
- dried fruits, berries, fruits with pulp or seeds
- foods containing sulfur or sulfate
- foods high in fiber, including whole-grain products
- hot sauce, pepper
- meats
- nuts, crunchy nut butters
- popcorn
- products containing sorbitol (sugar-free gum and candies)
- raw vegetables
- refined sugar
- seeds
- spicy foods, sauces
Types
There are many types of colitides. They are usually classified by the etiology.
Types of colitis include:
Autoimmune
- Inflammatory bowel disease.
Idiopathic
Iatrogenic
Vascular disease
Infectious
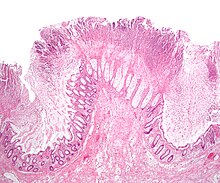
- Infectious colitis,
A well-known subtype of infectious colitis is pseudomembranous colitis, which results from infection by a toxigenic strain of Clostridium difficile (c-diff).[2]
Enterohemorrhagic colitis may be caused by Shiga toxin in Shigella dysenteriae or Shigatoxigenic group of Escherichia coli (STEC), which includes serotype O157:H7 and other enterohemorrhagic E. coli.[3]
Parasitic infections can also cause colitis.
Waste-basket
- Atypical colitis
Severity of colitides
- Fulminant colitis.
Any colitis with a rapid downhill clinical course[clarification needed] is known as fulminant colitis. In addition to the diarrhea, fever, and anemia seen in colitis, the patient has severe abdominal pain and presents a clinical picture similar to that of septicemia, where shock is present. Approximately half of these patients require surgery.
Irritable bowel syndrome, a separate disease, has been called spastic colitis or spastic colon. This name causes confusion, since colitis is not a feature of irritable bowel syndrome.
Treatment
How a given colitis is treated is dependent on its etiology.
Treatment of colitis may include the administration of antibiotics, Azathioprine or similar immunosupressants; steroids such as prednisolone and prednisone; one or several of a number of other drugs that ameliorate inflammation and pain (buscopan). As it is a chronic condition the objective is "remission" rather than cure.
Surgery is required only when the patient suffers from regular or permanent flare ups, especially in cases of fulminant colitis. Surgery usually entails removing the colon and bowel and creating a "pouch" with a portion of the small intestine, which in time adopts the characteristics of the colon.
Medical opinion is divided on the role of diet in colitis and IBD. Anecdotally, some sufferers find a change in diet can be effective at treating the symptoms of colitis and easing the side effects.[4] These can include reducing the intake of complex carbohydrates, refined sugar, lactose products, soft drinks, caffeine, and spicy foods.
See also
Notes
- ^ "Creating an Ulcerative Colitis Diet Plan". WebMD, LLC. Retrieved 2008-12-13.
{{cite web}}: Cite has empty unknown parameter:|coauthors=(help) - ^ "Clostridium Difficile Colitis - Overview". WebMD, LLC. Retrieved 2006-09-15.
{{cite web}}: Cite has empty unknown parameter:|coauthors=(help) - ^ Beutin L (2006). "Emerging enterohaemorrhagic Escherichia coli, causes and effects of the rise of a human pathogen". J Vet Med B Infect Dis Vet Public Health. 53 (7): 299–305. PMID 16930272.
- ^ Geerling BJ, Dagnelie PC, Badart-Smook A, Russel MG, Stockbrügger RW, Brummer RJ (2000). "Diet as a risk factor for the development of ulcerative colitis". Am. J. Gastroenterol. 95 (4): 1008–13. doi:10.1111/j.1572-0241.2000.01942.x. PMID 10763951.
{{cite journal}}: CS1 maint: multiple names: authors list (link)
External links
- Crohn's & Colitis Foundation of Canada
- Crohn's & Colitis Foundation of America
- The National Association for Colitis and Crohn’s Disease (UK)
- Blog for people suffering from Colitis.
- "Colitis". GPnotebook.
- Ulcerative Colitis, National Digestive Diseases Information Clearing House, National Institutes of Health (in the public domain)
- Ulcerative Colitis at Curlie
